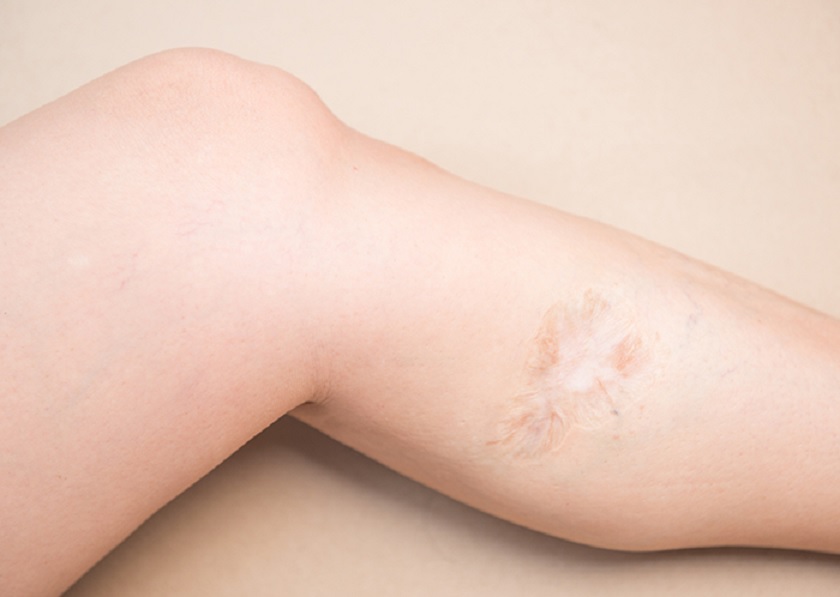
 Scar Revision in Nagpur plays an important role in the correction of scars and defects on the body surface. The final look is a concern.
Scar Revision in Nagpur plays an important role in the correction of scars and defects on the body surface. The final look is a concern.
Scar Treatment in Nagpur
Healing is a natural process of repairing damaged organic tissues that occurs through the production of collagen fibers. The scar is a definitive mark and one of the main concerns is its final appearance after cosmetic plastic surgery or repair plastic surgery to correct scars and defects. Even examining the patient’s skin type and surgical history, there is no way to be sure about the development of a pathological or unsightly scar.
Factors that influence the quality of scars
Location in the body
Certain body regions are at greater risk of developing scar changes (examples: anterior chest, shoulders, back, earlobes).
Scar shape
Oblique scars or scars with curved paths tend to have worse aesthetic results.
Wound direction in relation to lines of tension
Wounds that are not parallel to the lines of lesser tension in the skin can cause scars that are more tense and enlarged.
Wound size
Larger, deeper wounds with great loss of substance are more likely to have scar changes.
Age of patients
Young patients are more likely to have more visible scars than older patients.
Genetic characteristics
Patients with a dark color or of oriental origin are at greater risk of developing pathological scars.
Surgical technique
Adequate closure by planes, relieving the tension of the wound edges, tends to produce scars of better quality.
Postoperative care
Postoperative care reduces the risk of stitches opening or wound infection, contributing to good scar quality.
Healing time
Scars usually get less noticeable over the years.
Types of scar changes
Hypertrophic scar
Elevated scar that does not go beyond the limits of the initial wound, caused by disordered collagen production. It has a tendency to regress over time and is not hereditary.
Keloid
Elevated scar that extends beyond the limits of the initial wound, caused by excessive collagen production (behavior similar to a benign tumor). It does not tend to regress over time and is hereditary.
Retracted scar
Tense scar, which pulls the adjacent tissues (scar contracture, retractable or contractile scar). It can restrict normal movements of the affected area.
Elongated scar
Shallow, loose and spreading scar. It may result from increased tension on the sides of the scar or from rupture of stitches and healing by secondary intention.
Atrophic scar
Scar deeper than the relief of the surrounding skin. Among its causes, we can mention very thin skin and healing disorders due to metabolic diseases and nutritional deficiencies.
Dyschromic scar
Scar that is darker (hyperchromic) or lighter (hyperchromic) than the surrounding skin. Hyperchromia is more common and can be the result of sun exposure in a recent scar, especially in dark-skinned people.
Scar “in trapdoor”
A scar with a curved path (in a “C” or “U” shape), which causes the skin contained in its inner part to become more swollen due to the damming of lymphatic fluid.
Surgical Scar Treatment in Nagpur
Fusiform resections
• Direct resection, with primary closure whenever possible. Indication: short scars.
• Serial resections or skin expansion and subsequent resection. Indication: very wide scars.
• Intralesional resection by removing a scar spindle inside the lesion, reducing its width and thickness, without running the risk of creating new lesions. Indication: treatment of keloids.
Reorientation of scars
• W-plasty: removal of the old scar with wound closure with broken lines. It is indicated in wide scars or with stitch marks resembling train tracks, to dissipate the forces of contracture and prevent new scar retractions.
• Z-plasty (zetaplasty): making new incisions on each side of the old scar and creating small triangular flaps; transposition (reorientation) of the flaps to cover the wound, creating a “Z” or “zig-zag”. It is indicated to reposition and lengthen scars such as joints in joints (example: fingers, armpits, elbows), scars contrary to lines of lower tension (example: longitudinal scars on limbs) and “trapdoor” scars.
Defect correction
Facial and body contour defects can be acquired or congenital. The restorative procedures performed by plastic surgery to correct defects include:
• Treatment of injuries and sequelae caused by trauma resulting from previous surgeries, accidents, falls, aggressions, sports activities, burns, radiation, etc.
• Treatment of sequelae caused by tissue damage, such as varicose ulcers, ischemic ulcers, pressure or decubitus ulcers, etc.
• Treatment of sequelae caused by tissue infection.
• Treatment of wounds resulting from the removal of tumors or other injuries.
• Treatment of congenital anomalies, involving morphological and structural changes in terms of shape, size, etc.
Surgical treatments for defects
Wound closure
• Primary closure (first intention): approximation of the wound edges with sutures. It presents rapid epithelialization and minimal formation of granulation tissue.
• Secondary closure (spontaneous or by second intention): wounds are left open. Debridement of devitalized tissue using antibiotics, dressings, and frequent wound care are necessary. Closure is slow and depends on the contraction generated by the healing process.
• Delayed primary closure (third intention): wounds are left open initially and, after a few days, are closed with sutures.
• Elastic suture: alternative treatment for closing large wounds. Elastic rubber bands are sutured under moderate tension on the edges of the wounds, promoting their gradual approximation until their complete closure.
Grafts
Grafts are tissues transferred from a donor area to a recipient area, without maintaining its vascular pedicle, thus, the recipient area must be well vascularized so that the grafted tissue, through intimate contact, integrates. Several tissues can be grafted, including: skin, mucosa, hair (hair transplant), fat (fillers), muscle fascia, bones, cartilage, tendons, nerves and vessels.
Grafts can consist of a single type of tissue, for example, skin (single grafts) or more than one type, for example, a fragment of skin with cartilage taken from the ear for reconstruction of nasal defects (compound grafts). Skin grafts can be partial or full thickness and are very useful in closing large wounds.
Patchwork
Flaps are tissues transferred from a donor area to a recipient area, with maintenance of their vascular pedicle (definitive or temporary), that is, in principle, they have their own circulation, regardless of the recipient area. They are indicated for the closure of larger wounds (examples: defects after tumor removal and wounds that do not close by simply approaching the edges of the lesion), reconstruction of more complex structures (examples: nose and ear reconstruction), coverage of structures (examples: coverage of vessels, bones and cartilage) and areas with vascular deficiency or bony protrusions (examples: areas without a bed for graft integration and pressure ulcers).
The flaps may be local, regional or distant, and may contain skin, subcutaneous tissue and muscle. They can have different shapes, such as: tubes, spindles, triangles, rectangles, etc. They can also be divided into random (randomized) flaps, which present vascularization without a defined anatomical path, and axial (arterial) flaps, which present vascularization based on the anatomical location of a known artery. Random flaps are transferred through advances, rotations, interpolations, among other ways, while axial flaps are transferred in an island, peninsula or free (microsurgical).
Expansores
Expansion is indicated when there is not enough skin to repair defects. Its results are aesthetically superior in relation to the transfer of flaps from other regions, which may have different color, texture and capillary coverage. The procedure is performed using a silicone expander balloon inserted under the skin or muscle, close to the area to be repaired. The expander is gradually filled with saline over weeks to months, causing the local skin to stretch and grow.
Examples of some of its applications are:
(1) breast reconstruction : when there is not enough skin to accommodate a silicone implant and
(2) head and neck reconstruction : when there is not enough skin tissue to cover areas of the face, neck or scalp, where hair growth makes it difficult to replace lost tissue with skin from other regions.
Expansion may be difficult in areas where the skin is thicker, such as the back. If the area to be expanded is damaged and inelastic scarring, this procedure is probably not a good option.
Implants
The basic difference between implants and prostheses is that the implant is included within regions of the body, while the prosthesis, even when fixed, is only fitted. Implant is the correct term for most silicone products and other alloplastic materials used in plastic surgery, however, the term prosthesis has become very popular and is used practically synonymously.
The increase in volume and the definition of contour provided by the implants make them also very useful in reconstructive surgeries, such as:
(1) head and neck reconstruction : cartilaginous grafts used in nose and ear reconstructions, for example, can be replaced in some cases by pre-molded silicone parts,
(2) breast reconstruction : the breast implant creates or reestablishes the contour of the breast, providing volume and projection under the local tissue or below a myocutaneous flap transferred to the region,
(3) reconstruction of the pectoral region : the pectoral implant can correct traumatic or congenital asymmetries of the region,
(4) reconstruction of the calves: the calf implant can symmetrize defects resulting from sequelae of infantile paralysis, trauma or genetic anomalies that affect the legs.
COMMON QUESTIONS
What options are there for scar treatment in Nagpur?
- Compressive dressings
- silicone plates
- Use of ointments and massages
- Surgical treatment
- Corticosteroid injection
- Beta therapy (use of radiation at the scar site)
- Others
What drives people to seek scar revision in Nagpur?
The search is based on 2 aspects: making the scar more aesthetically pleasing and improving the function of the compromised area.
Will my scars fade?
We can make them less noticeable, but they will never really disappear.
Can my skin colour influence healing?
Normally, light-skinned individuals are less likely than dark-skinned people or people of oriental descent to develop any type of unsightly scarring, regardless of the type of technique used.
What is the best time to start scar treatment in Nagpur?
Normally, we do not perform scar corrections before 6 months to 1 year of scar existence, due to the intense process of evolution through which it can go.
Will I have a keloid or hypertrophic scar again?
In both situations the lesions can return, and this is much more frequent in the case of keloids.
Will I feel pain after surgery?
Usually not, but occasionally pain may occur, which is most often associated with movement of the operated area, and which usually subsides with common analgesics.
What type of anesthesia is used?
Normally, local anesthesia is used, but in cases of very extensive scars or in very anxious patients, sedation can be used. In some special cases, other types of anesthesia may be used.
How long will my surgery last?
It can last from a few minutes to hours, depending on the size of the scar to be corrected. During the surgical procedure, newsletters about the surgery and the patient’s condition may be issued periodically, if the family wishes.
How long will I be hospitalized?
The patient may be released immediately after the surgery, he may have to wait a few hours or may only be released the next day, depending on the type of anesthesia to be used.
Will dressings and drains be used in my surgery?
Yup. Dressings may be simple or compressive, depending on the type of surgery. Drains are used only in some cases where there is a large detachment of the skin.
Are there stitches to be removed?
Sometimes yes, depending on the type of wire used. When necessary, they are withdrawn Between the 7th. and the 15th. postoperative day, and must be strictly performed by my team.
When can I return to my physical activities?
It depends on the type of exercises and individual evolution, there is no standard period. Heavy exercises involving the operated area should wait at least 1 month, depending on the case.
How long after surgery is the final result achieved?
Only after the 12th month will the scar reach its definitive shape.
Are there any risks of complication in this type of surgery?
Scar correction is usually safe, but there is always the possibility of complications. These can include infection, bleeding, a reaction to anesthesia, or the return of an unsightly scar.
When will I be able to shower at the surgery site?
Depending on the case, even the day after the surgery. Everything will depend on the evolution of your surgery, as well as the type of dressings, observing only the special care that will be taught by your doctor.
How is the postoperative evolution?
You must not forget the 12 months required to achieve the desired result. Until then, any and all concerns on your part should be transmitted to your doctor, who will provide you with the necessary clarifications for your peace of mind.
Should the sun be avoided?
For a period of 30 days, after which exposure to the sun should be gradual, using sunscreen.
Is there sensitivity modification?
There may be a small change in sensitivity in the first two months or so, which gradually disappears.
Is the result rewarding?
If you are aware of what you want and the surgeon can provide you with what you asked for, it certainly pays off. However, it is important to take into account the fact that some types of scars do not have such a good evolution, and can present difficult and time-consuming treatment.
