Patient Education Guide · Dr. Bhupendra Gaidhane
A plain-language guide from a Nagpur plastic surgeon — for the man who’s been avoiding the mirror, the gym, or the beach for far too long.
“Doctor, I thought it would go away on its own. My family said it’s normal. I kept waiting.”
I understand. Gynecomastia is one of those conditions that carries a lot of shame and very little conversation. So men wait. They wear dark, loose shirts. They skip swimming. They avoid the gym locker room. And by the time they sit across from me, they’ve been quietly suffering — often for 5 to 10 years.
Here’s what I want you to take from this article: the grade of your gynecomastia determines everything — the surgical technique, how big the scar will be, how long recovery takes, and what the final result looks like. And the higher the grade, the more complex all of those things become.
This isn’t scare-mongering. This is simply the biology of the condition. Skin that hasn’t been stretched yet has elasticity. A gland that’s small is easier to remove cleanly. An incision on fresh, tight skin heals beautifully. Once that window passes — once the skin starts to sag and stretch — you’re in a different category of surgery entirely.
Let me walk you through each grade, exactly as I explain it to patients sitting in front of me.
Gynecomastia is now India’s 5th most common cosmetic surgery. In 2024 alone, over 47,000 Indian men had the surgery — a 10.8% jump from the year before. 94% of India’s plastic surgeons perform this procedure. You are far from alone.
Many patients first struggle to understand whether the issue is fat or gland. You can read a detailed explanation here → Chest Fat vs Gynecomastia: How to Tell the Difference
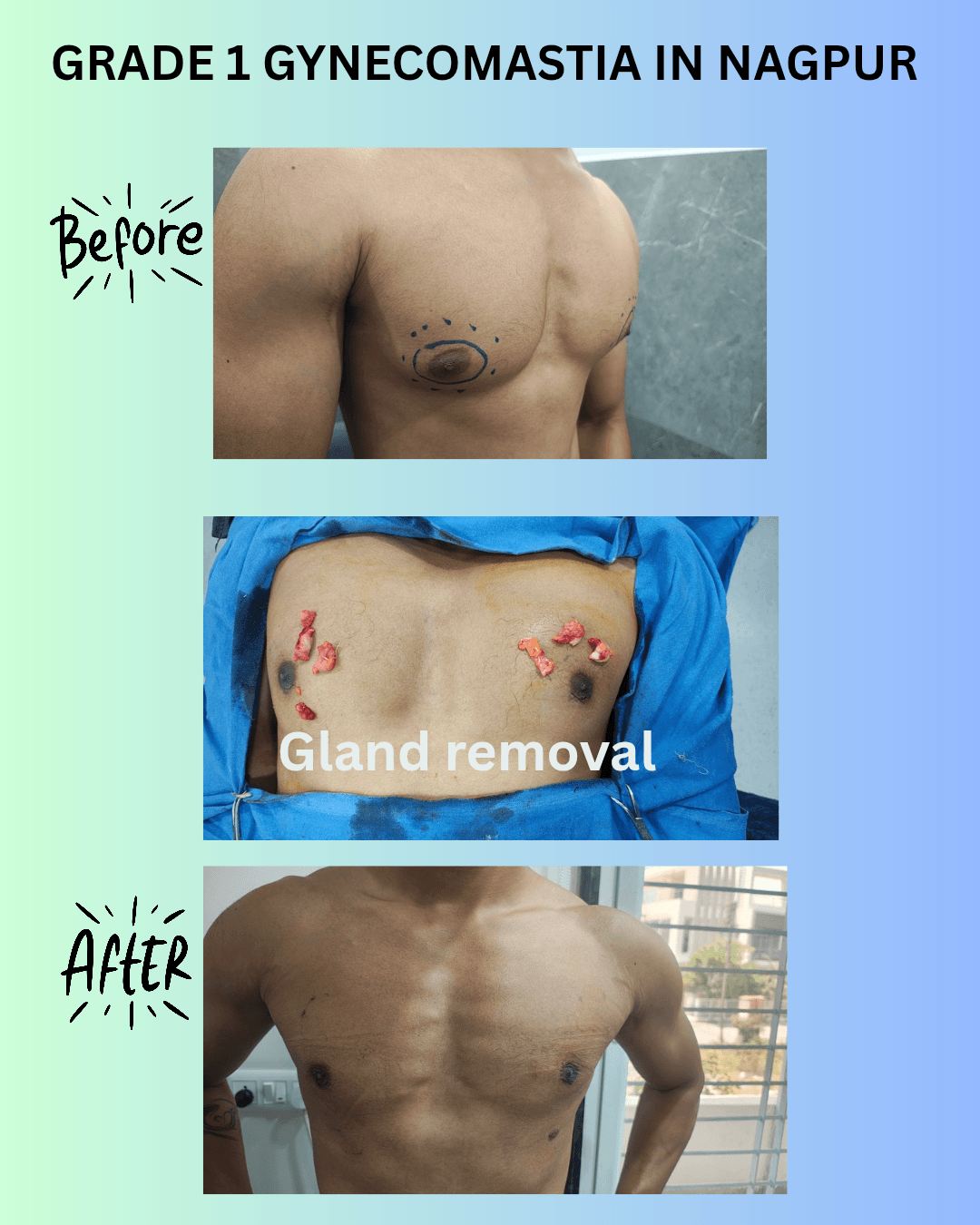
Grade 1 — “Puffy Nipples”
The Earliest, Most Treatable Stage
Grade 1 Gynecomastia
Small subareolar gland · No skin excess · Excellent surgical outcome
Patient example: Subareolar fullness / puffy nipple — pre-op and 3-month post-op
This is the grade most men don’t even know they have. There’s no obvious “breast” — what you see is the nipple area looking slightly puffy, almost like it’s been pushed outward from behind. In medical language, we call it subareolar fullness.
“In clinic, I ask the patient to lie on his back. I place two fingers just behind the nipple. If I feel a firm, rubbery disc — sometimes the size of a 10-rupee coin — that’s the gland. That’s Grade 1. Most patients are shocked. They thought it was just fat.”
Grade 1 gynecomastia is almost always pure glandular tissue — there’s very little fat involved. The gland is small, confined to the area directly behind the nipple-areola complex, and the skin overlying it is completely normal — tight and elastic.
Each grade reflects differences in gland, fat, skin excess, and nipple position, which directly influence treatment planning
What Grade 1 looks and feels like:
- Nipples appear “puffy” or protruding — especially noticeable in a tight t-shirt
- You can feel a hard or rubbery disc behind the nipple when you press
- Sometimes tender or sensitive, especially in teenagers
- Usually affects both sides, though one side may be slightly larger
- Not visible when wearing clothes, but very obvious shirtless
- Chest otherwise looks flat and normal
I use micro-incision gland excision through a tiny 4–5 mm incision placed right at the lower edge of the areola — where the skin naturally changes colour. The scar fades into this border within a few months and becomes virtually invisible. At Grade 1, the enlargement is purely glandular with little to no fat — so liposuction is not needed. This is a day-care procedure. You go home the same afternoon.
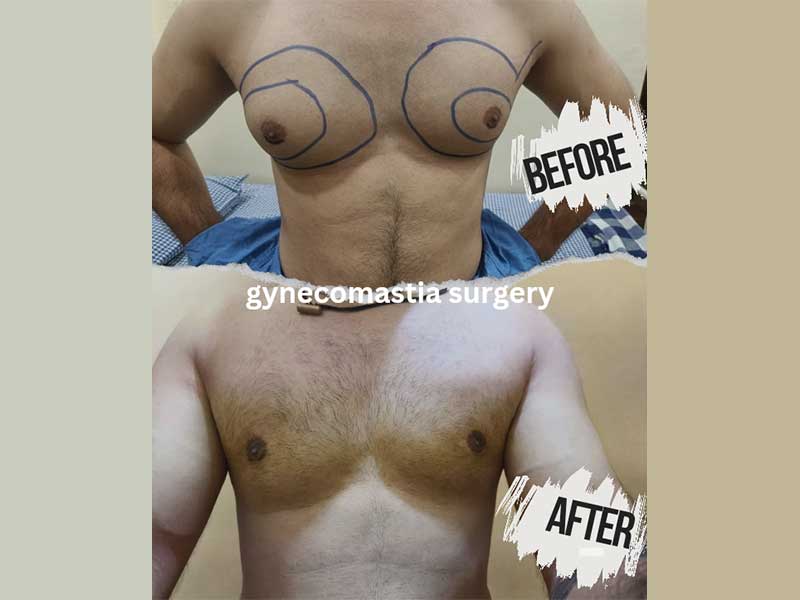
Grade 2 — Visible Chest Enlargement
The Grade I See Most Often in Nagpur
Grade 2 Gynecomastia (2a & 2b)
Moderate enlargement extending beyond areola · Skin still has good elasticity
Patient example: Grade 2a (no skin excess) and Grade 2b (minor skin excess) — pre-op and 3-month post-op
Grade 2 is by far the most common presentation I see. The chest has a clear, rounded shape that’s visible even through a shirt. When the man removes his shirt, there’s an obvious “breast-like” mound — not as dramatic as a female breast, but unmistakeable. This is what men are typically referring to when they say they have “man boobs.”
Grade 2 is divided into two subtypes:
- Grade 2a — moderate enlargement, but the skin is still tight and there’s no excess hanging skin
- Grade 2b — slightly more tissue, and the skin has started to show very minor laxity
“The difference between 2a and 2b matters because it tells me how the skin will behave after I remove the tissue. In 2a, the skin retracts beautifully on its own with VASER. In 2b, I sometimes need to take a slightly more careful approach to ensure the skin sits flat. But in both cases — no skin removal, no major scars.”
At this grade, there’s usually a mix of both glandular tissue and fat. That’s why VASER liposuction combined with gland excision works so well here. The VASER energy helps the skin retract after fat removal — something conventional liposuction cannot do as effectively.
Early stages are easier to manage and often require less extensive intervention compared to advanced grades.
Gynecomastia Treatment Options in Nagpur
What Grade 2 looks and feels like:
- Chest mound clearly visible in fitted clothes or gym wear
- Breast tissue extends beyond the areola, towards the sides of the chest
- Both a soft component (fat) and firm component (gland) when touched
- Visible and prominent when shirtless
- Nipple may appear to point slightly downward or forward
- Many patients have mild tenderness
From Grade 2 onwards, fat removal becomes part of the surgery. Standard liposuction works — but Lipovase, the 4th generation VASER technology I use, goes significantly further. It is the most advanced ultrasound-assisted liposuction available in Central India, and the only technology I use for male chest contouring.
Lipovase (4th-gen VASER) + micro-incision gland excision. The VASER precisely emulsifies and removes the fat component, while its ultrasound energy simultaneously stimulates the skin to contract. The gland is excised through the same tiny 4–6 mm incision at the areola border. Result: a flat, masculine chest with a near-invisible scar. Day-care surgery — home the same evening. Base cost ₹60,000; with Lipovase upgrade ₹80,000.
Grade 3 — Moderate Enlargement
When the Skin Starts to Lose Its Snap
Grade 3 Gynecomastia
Significant enlargement · Skin laxity present · Surgery more complex
Patient example: Grade 3 with moderate skin excess — pre-op and 6-month post-op
By Grade 3, the breast enlargement is significant. The tissue has expanded beyond just the nipple area — it fills out across the lower chest, creating an obviously feminine breast shape. More importantly, the skin has now been stretched over time and has started to lose its elasticity.
This is the grade where I have a very honest conversation with my patients. I say: “We can still get an excellent result, but the surgery is more involved than if you’d come to me two years ago.”
“With Grade 3, the key challenge is the skin. After I remove all that tissue, the skin needs to retract and sit flat on the chest wall. VASER helps this a great deal — it preserves the deep connective tissue that helps the skin ‘zip up’. In many Grade 3 patients, we still avoid skin excision. But in some — particularly heavier patients, or those who’ve had the condition for many years — a small skin resection becomes necessary. I always explain this before surgery, never as a surprise.”
What Grade 3 looks and feels like:
- Prominent chest mound visible from a distance, even in a loose shirt
- Breast tissue extends towards the armpit (lateral chest)
- Skin may feel slightly loose or “floppy” rather than taut
- Nipple-areola complex may begin to droop slightly downward
- Significant emotional impact — many patients at this grade are deeply self-conscious
- Often associated with weight gain or obesity
At Grade 3, whether or not you need skin removal depends heavily on your individual skin quality, age, BMI, and how long you’ve had the condition. Younger patients with good skin elasticity can often avoid skin resection even at Grade 3 — and Lipovase VASER’s active skin-tightening effect significantly improves the chances of avoiding skin excision. This is why I strongly recommend the Lipovase upgrade for all Grade 3 patients. This is also why I insist on an in-person clinical examination before discussing the surgical plan. A photo or a WhatsApp message cannot tell me how your skin will behave.
Grade 4 — Severe Enlargement
The Grade Where Scars Become Unavoidable
Grade 4 Gynecomastia
Female-pattern breast appearance · Significant skin excess · Skin resection typically required
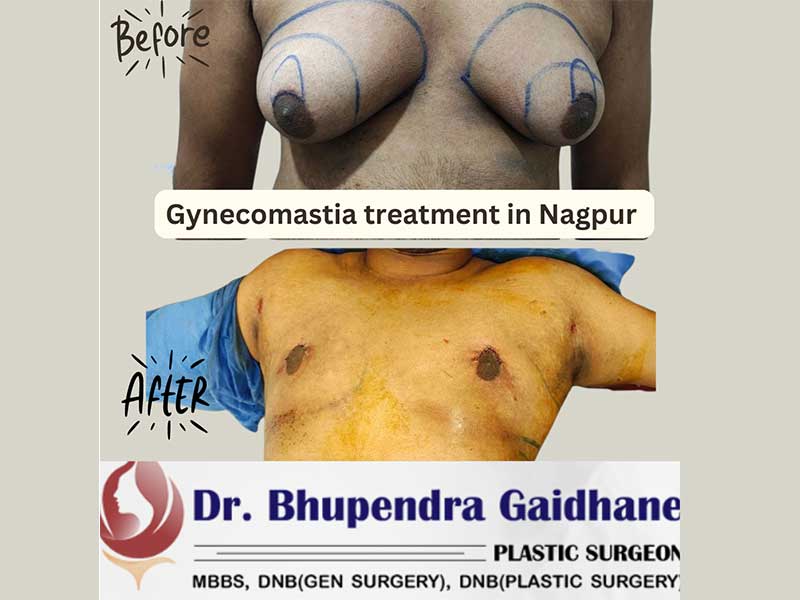
Patient example: Grade 4 with significant ptosis and skin excess — pre-op and on table post-op
Grade 4 is the most advanced stage of gynecomastia. The chest now closely resembles a female breast — there is substantial volume, the nipple-areola complex has drooped downward (what surgeons call ptosis), and there is a significant amount of excess skin hanging from the lower chest. These patients typically also have significant amounts of fat alongside the glandular tissue.
I want to be very direct with Grade 4 patients: this surgery will leave a more visible scar. To achieve a flat, masculine chest, I have to remove not just the tissue but also the excess skin. There is no way around this. The technique is similar to a breast reduction procedure — we create a scar that runs along the lower border of the chest or around the areola.
“I tell Grade 4 patients: you have two choices. We do thorough surgery that removes everything and gives you a flat chest with a visible but well-placed scar. Or we do minimal surgery that reduces the size but leaves skin laxity and an imperfect result. Almost every patient chooses the first option. A scar you can’t see in a shirt is better than breasts you can.”
The good news: even at Grade 4, the surgery is very effective, and results are life-changing. Patients who come to me at Grade 4 often say the improvement in their confidence and daily life is enormous — worth every day of recovery.
Higher grades often involve excess skin and require a more structured surgical approach
What Grade 4 looks and feels like:
- Large, visibly feminine-shaped breasts — clearly apparent even fully clothed
- Nipple-areola complex pointing downward, sometimes towards the belly
- Significant excess skin, especially at the lower chest and under the breast
- Deep emotional and social impact — many patients have completely withdrawn from social activities
- Often seen in patients who have lost significant weight, or who have had the condition for 10+ years
- Chest skin feels stretched, thin, and has poor rebound when pinched
Even at Grade 4, my goal is to place scars in the most concealed locations possible — along the lower border of the chest, within natural skin folds, and around the areola margin. Lipovase VASER is used as standard at this grade to remove fat with maximum precision and minimal trauma before skin resection. Scars mature and fade significantly over 12–18 months with silicone scar therapy. The final result, while more complex to achieve, can still be genuinely life-changing.
Grade-by-Grade Comparison:
Surgery, Scars & Recovery at a Glance
Here’s the honest, practical breakdown of what each grade means for your surgery — the information I give every patient before they go to the operation theatre:
| Factor | Grade 1 | Grade 2 | Grade 3 | Grade 4 |
|---|---|---|---|---|
| Skin Removal Needed? | No | No (2a) / Rarely (2b) | Sometimes | Usually Yes |
| Scar Size | 4–5 mm, invisible | 4–6 mm, minimal | Moderate | Larger, well-placed |
| Surgery Complexity | Simple | Moderate | Involved | Complex |
| Anaesthesia | Local / sedation | GA / sedation | General (GA) | General (GA) |
| Hospital Stay | Day care | Day care | Day care / 1 night | 1 night (sometimes) |
| Back to Work | 2–3 days | 3–5 days | 5–7 days | 7–14 days |
| Full Recovery | 4–5 weeks | 5–6 weeks | 6–8 weeks | 10–12 weeks |
| Base Surgery Cost | ₹50,000 | ₹60,000 | ₹70,000 | Up to ₹90,000 |
| Lipovase VASER Add-on | Not needed | + ₹20,000 (optional) | + ₹20,000 (recommended) | + ₹20,000 (standard) |
| Result Quality | Excellent | Excellent | Very Good | Good (scar trade-off) |
| Grade | Base Cost | + Lipovase VASER | Surgical Complexity |
|---|---|---|---|
| Grade 1 | ₹50,000 | Not required | Small gland only · No fat component |
| Grade 2 | ₹60,000 | + ₹20,000 | Moderate gland + fat · VASER optional |
| Grade 3 | ₹70,000 | + ₹20,000 | Larger gland · Chest contouring required |
| Grade 4 | Up to ₹90,000 | + ₹20,000 | Advanced · Possible skin procedures |
*All costs are indicative. Final cost confirmed after in-person examination based on grade, technique, and individual anatomy. Source: Gynecomastia Surgery Cost Nagpur 2026
Why Operating Early is Always the Smarter Decision
This is the section I wish every young man with gynecomastia would read. Because the single biggest factor that determines how simple or complex your surgery is — how big the scar will be, how long recovery takes, how good the final result looks — is how long you’ve waited.
1. Early = No skin removal, no major scars
At Grade 1 and Grade 2a, the skin hasn’t been stretched. After I remove the tissue and fat, the skin contracts beautifully on its own — especially with VASER technology. You end up with a flat chest and a scar that’s literally the size of a small puncture wound, hidden at the edge of the areola. Most people cannot find it at the 3-month review.
At Grade 3 and 4, the skin has been stretched for years. It no longer has that elastic rebound. When I remove the tissue, the skin doesn’t fully retract. That’s when skin resection — with its larger, more visible scars — becomes necessary.
2. Early = Lower cost
Simpler surgery = shorter operation time = lower surgical fees, lower anaesthesia charges, and no hospital overnight stay. A Grade 1 surgery typically costs roughly half of what a Grade 4 surgery costs. The condition doesn’t get cheaper to treat by waiting.
3. Early = Faster recovery
Grade 1 and 2 patients are typically back at their desk in 2–3 days. Grade 4 patients may need 10–14 days off work, and 10–12 weeks before they can return to full gym activity. Early surgery means minimal disruption to your life.
4. Early = Better skin quality over the implant
When the underlying architecture is correct — tissue removed cleanly, fat contoured with VASER, skin allowed to retract naturally — the skin drapes beautifully over the chest muscles. The result looks like you simply have a flat, athletic chest. Not “someone who had surgery.” At higher grades, even with excellent surgery, there can be residual contour irregularities as the stretched skin settles.
5. Early = Younger skin heals better
Skin in your late teens and early twenties has maximum collagen density and vascularity. Scars heal faster, fade more completely, and skin contracts more reliably. If you’re reading this at 17, 18, or 21 — this is your golden window. Don’t wait for it to close.
“I had a 27-year-old patient last month — Grade 2a, flat chest the next morning, back to his IT job in three days, a tiny scar hidden at his areola edge that you’d need a magnifying glass to find. He told me he’d been suffering since age 16. Eleven years. For a surgery that took 75 minutes and changed his life. Please don’t let that be you.”
Pubertal gynecomastia can spontaneously resolve — but only within the first 1–2 years after onset. If you still have it by age 18 or 19, the chances of it resolving without surgery are very small. The gland hardens over time, becoming fibrous. No exercise, no medication, no supplement can remove a hardened glandular disc. Only surgery can.
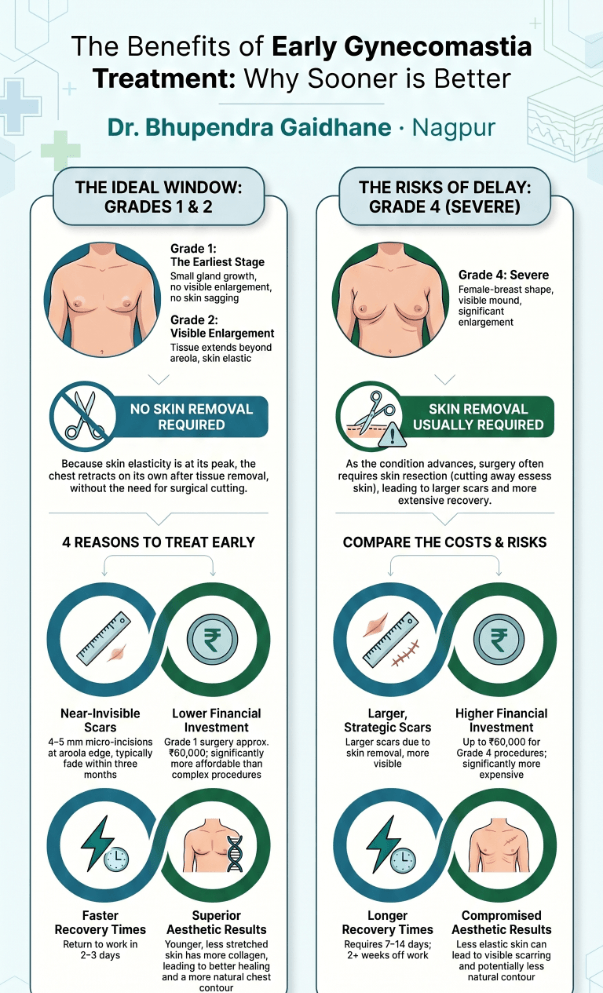
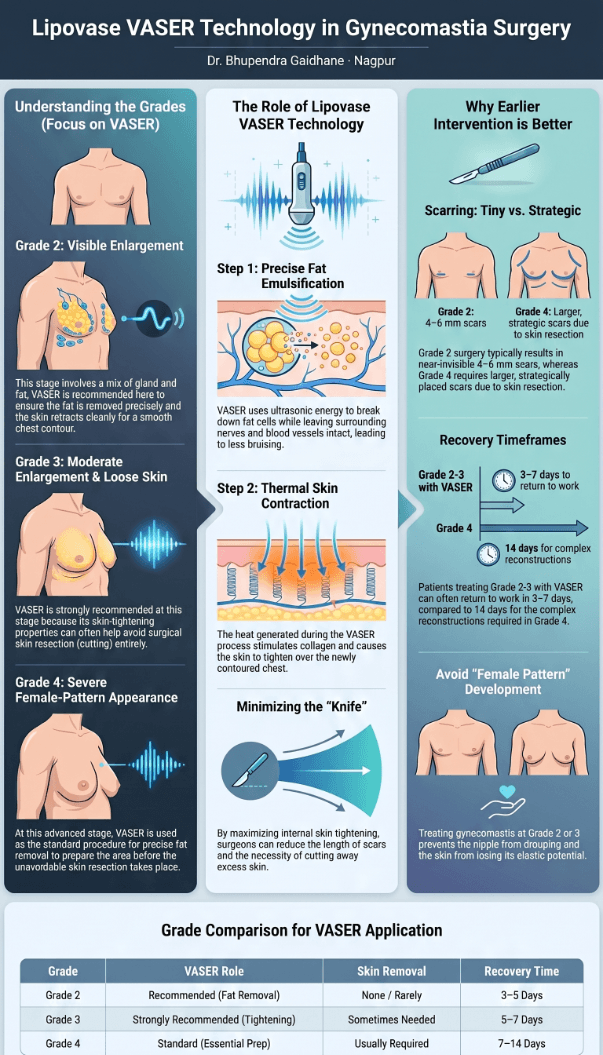
Visual Summary: The 4 Grades of Gynecomastia
The infographic below summarises everything we’ve discussed — print it, save it, share it with someone who needs to read this.
These are the questions I get asked most often in clinic and on WhatsApp. Honest answers only.
You can get a rough idea from photos and descriptions, but accurate grading requires a physical examination. The pinch test (pressing the fingers behind the nipple to feel the gland), assessment of skin laxity, and measurement of tissue volume are all done in person. I always grade the patient myself before discussing the surgical plan — photographs on a phone are not enough.
If the Grade 1 gynecomastia has been present for more than 12–18 months and you’re past puberty, it is very unlikely to resolve on its own. Waiting only risks progression to Grade 2. Grade 1 surgery is the simplest, fastest, cheapest, and gives the best cosmetic result. There is no clinical reason to delay once you are physically mature and emotionally ready.
All surgery involves some form of incision. At Grade 1 and 2, my incisions are 4–6 mm, placed at the lower edge of the areola where the natural colour change hides the scar line. At 3–6 months, these scars are typically near-invisible. At Grade 3 and 4, where skin removal is sometimes needed, scars are larger but are placed in the most concealed positions possible. I use layered closure techniques and recommend silicone scar sheets post-operatively for all patients.
Because true gynecomastia involves glandular tissue — not fat. No amount of chest pressing, bench pressing, or cardio can remove a glandular disc. Exercise can reduce the fat component around it, which sometimes makes the gland more noticeable (not less). If there’s a firm lump behind the nipple, that’s gland — and only surgery removes it.
I operate on patients from age 16 upward, as long as they’ve had the condition for at least 12–18 months and it’s not regressing. Below 16, I usually recommend observation unless the psychological impact is very significant. The ideal age window is 17–25 — when skin elasticity is at its highest and recovery is fastest.
Once the glandular tissue is properly excised, it does not regenerate. Recurrence is rare — it typically only occurs if a hormonal abnormality is left untreated, or if anabolic steroids are used post-surgery. The fat component can return with significant weight gain, but the gland will not. The surgery is considered permanent.
The surgery itself is performed under anaesthesia — you feel nothing. Post-operatively, there is some tightness and mild discomfort in the chest for the first 3–5 days, well managed with prescribed pain relief. Most patients describe it as a “tight, sore” feeling rather than sharp pain. By Day 5–7, most patients are comfortable enough to not need any painkillers.
Chest fat (pseudogynecomastia) is soft, uniform, and spreads across the entire pectoral area — it responds to weight loss and exercise. True gynecomastia has a firm or rubbery disc of tissue directly behind the nipple — you can feel it distinctly when you press. Many men have a combination of both. The easiest test: lie flat and press two fingers firmly behind your nipple. If you feel a hard button-like mass, that’s a gland — that’s gynecomastia.
Not Sure Which Grade You Are?
Book a personal consultation. I’ll examine you, grade your gynecomastia, and give you an honest surgical plan — with transparent costs, no surprises.
- Chest Fat vs Gynecomastia: How to Tell the Difference
- Gynecomastia Surgery in Nagpur
- Gynecomastia Recovery Timeline
- Liposuction Treatment
Prime Polyclinic, Cabin No. 3, 1st Floor, Diamond One Building, Dhantoli, Nagpur · Mon–Sat 10am–7pm