Home ›
Blog ›
Liposuction vs Tummy Tuck
Liposuction vs Tummy Tuck: What’s the Real Difference — and What Do You Actually Need?
Plastic & Cosmetic Surgeon, Nagpur
Body Contouring
Clinically Reviewed
They come in saying: “My stomach doesn’t look like it used to — even after months at the gym.”
That frustration is valid. And the reason it persists is almost never lack of effort. It’s usually a structural problem that exercise simply cannot fix.
The abdomen is not a single structure. It has three separate layers — fat, skin, and muscle — and each one behaves completely differently. When you treat the wrong layer, you get an incomplete result. This is exactly where most patient disappointment begins.
This guide breaks down what liposuction and tummy tuck each correct, who genuinely needs which, and where combining both gives the most complete outcome. Three real patient scenarios are included to help you see yourself in the decision.
Why Three Layers Matter More Than One Procedure
Before comparing procedures, it is essential to understand why the abdomen is uniquely complex. Three distinct layers each require a different treatment approach:
The Three Abdominal Layers — and What Each Needs
This is why gym routines plateau. Exercise improves muscle tone and reduces overall fat — but it cannot tighten skin that has lost elasticity, and it cannot close a muscle separation that occurred during pregnancy. These are anatomical realities, not failures of effort.
What Liposuction Actually Does — and What It Never Will
Liposuction is a fat-removal procedure. It does not address skin or muscle. Understanding this boundary is what separates a good outcome from a disappointing one.
What liposuction corrects
- ✓ Localised fat deposits in the abdomen, flanks, and back
- ✓ Waist definition and overall body contour
- ✓ Love handles (flanks) and back fat rolls
- ✓ Mild contour irregularities where skin is still elastic
What liposuction does not do
- ✗ Does not remove or tighten loose skin
- ✗ Does not repair separated abdominal muscles (diastasis recti)
- ✗ Does not correct post-pregnancy structural changes
Lipovase (4th Generation VASER) — why precision matters
In my Nagpur practice, I use Lipovase (VASER technology) — not conventional liposuction. VASER uses ultrasound energy to selectively break down fat while preserving surrounding tissue. This means smoother contour transitions, better precision in sculpting, and more predictable results — particularly in 360° body contouring.
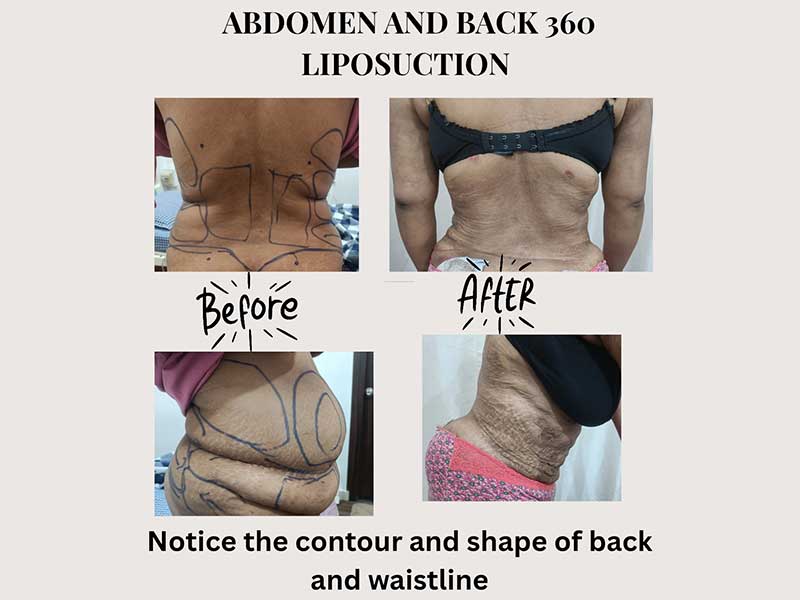
What is 360° liposuction?
Most patients focus only on the front abdomen. But the body is three-dimensional. Treating only the front can leave the waist appearing flat from the front but wide from the sides — an unbalanced result. 360° liposuction treats the abdomen, flanks, and back in a single session, creating a proportionate waistline visible from all angles. It remains, however, a fat-correction procedure — loose skin and muscle separation still require a tummy tuck if present.
What a Tummy Tuck Actually Corrects
Abdominoplasty (tummy tuck) is a structural restoration procedure — not a fat-removal surgery. Its purpose is to correct what fat removal alone cannot.
What a tummy tuck corrects
- ✓ Loose or hanging abdominal skin
- ✓ Muscle separation (diastasis recti) — the central abdominal gap
- ✓ Lower abdominal stretch marks (within the area of skin removed)
- ✓ Post-pregnancy abdominal changes involving all three layers
What a tummy tuck does not do
- ✗ Not designed for fat removal alone — liposuction handles fat
- ✗ Not a weight-loss procedure
Diastasis Recti — Why the “Mummy Tummy” Bulge Persists
The Post-Pregnancy Abdomen — Where Most Decisions Go Wrong
During pregnancy, three distinct changes occur simultaneously:
- Muscles stretch and often separate — creating diastasis recti, the central gap that causes the classic “mummy tummy” bulge that exercise cannot close
- Skin expands beyond its elastic limits — and does not fully retract after delivery, regardless of weight loss
- Fat distribution shifts — often accumulating in areas that are resistant to diet and exercise
Three Real Patient Scenarios
Procedure decisions are made on individual anatomy — not generalisations. These three scenarios represent common presentations seen at this practice in Nagpur.
Case Scenario 01
32-year-old woman, 14 months post-partum, persistent lower belly bulge
Situation: She delivered 14 months ago, reached near-pre-pregnancy weight, and has been consistent with gym and core workouts for 10 months. Despite this, she has a persistent lower abdominal bulge, visible loose skin, and some fullness in the flanks.
Clinical finding: Moderate diastasis recti (approx 3 cm gap), mild-moderate skin laxity, moderate fat in lower abdomen and flanks, good skin quality superiorly.
Case Scenario 02
28-year-old man, gym-going, stubborn fat in flanks — skin tight and elastic
Situation: Works out consistently, follows a structured diet, good physique overall — but stubborn fat in the flanks and lower back creates a boxy silhouette. No significant weight fluctuation. Skin pinch test confirms excellent elasticity.
Clinical finding: Localised fat in flanks, back, and lower abdomen. Skin tone excellent. No muscle separation. BMI normal.
Case Scenario 03
40-year-old woman, 28 kg weight loss, loose skin with residual fat
Situation: Lost 28 kg over 18 months through diet and exercise. However, the lower abdomen has loose, hanging skin and residual fat in the flanks. Skin shows significant stretch marks and poor elasticity.
Clinical finding: Significant skin excess (apron), residual fat in flanks and upper abdomen, mild diastasis, poor skin elasticity throughout.
Liposuction vs Tummy Tuck — Visual Comparison
Liposuction vs Tummy Tuck at a Glance
How to Know What You Actually Need
|
🔧 Liposuction only
|
📐 Tummy tuck only
|
📋 Both procedures
|
Recovery — Setting Realistic Expectations
|
Liposuction Recovery Days 1–3: Soreness and swelling — expected. Light activity possible. Week 1–2: Return to desk work. Avoid strenuous activity. Weeks 4–6: Compression garment throughout. Progressive improvement. 3–6 months: Final contour visible as swelling fully resolves. |
Tummy Tuck Recovery Week 1: Bed rest with assistance. Slightly bent posture is normal. Weeks 2–3: Gradual mobilisation. Light walking encouraged. Weeks 4–6: Most daily activities resumed. Core activities restricted. 3–6 months: Scar matures and softens. Final result visible. |
Why Patients in Nagpur Choose This Practice
- Layer-specific analysis — Every consultation distinguishes clearly between fat, skin, and muscle to identify the actual problem before any procedure is recommended
- Lipovase (VASER 4th Gen) technology — Used for all liposuction procedures, offering precision and smoother results than conventional liposuction
- No fixed packages — Procedures are planned case by case. A post-pregnancy patient and a gym-going male have fundamentally different needs
- Post-pregnancy specialisation — One of the most complex and underserved areas of body contouring in Nagpur
- Honest scar and recovery discussions — Before any decision is made, scars, timeline, and realistic outcomes are discussed in full
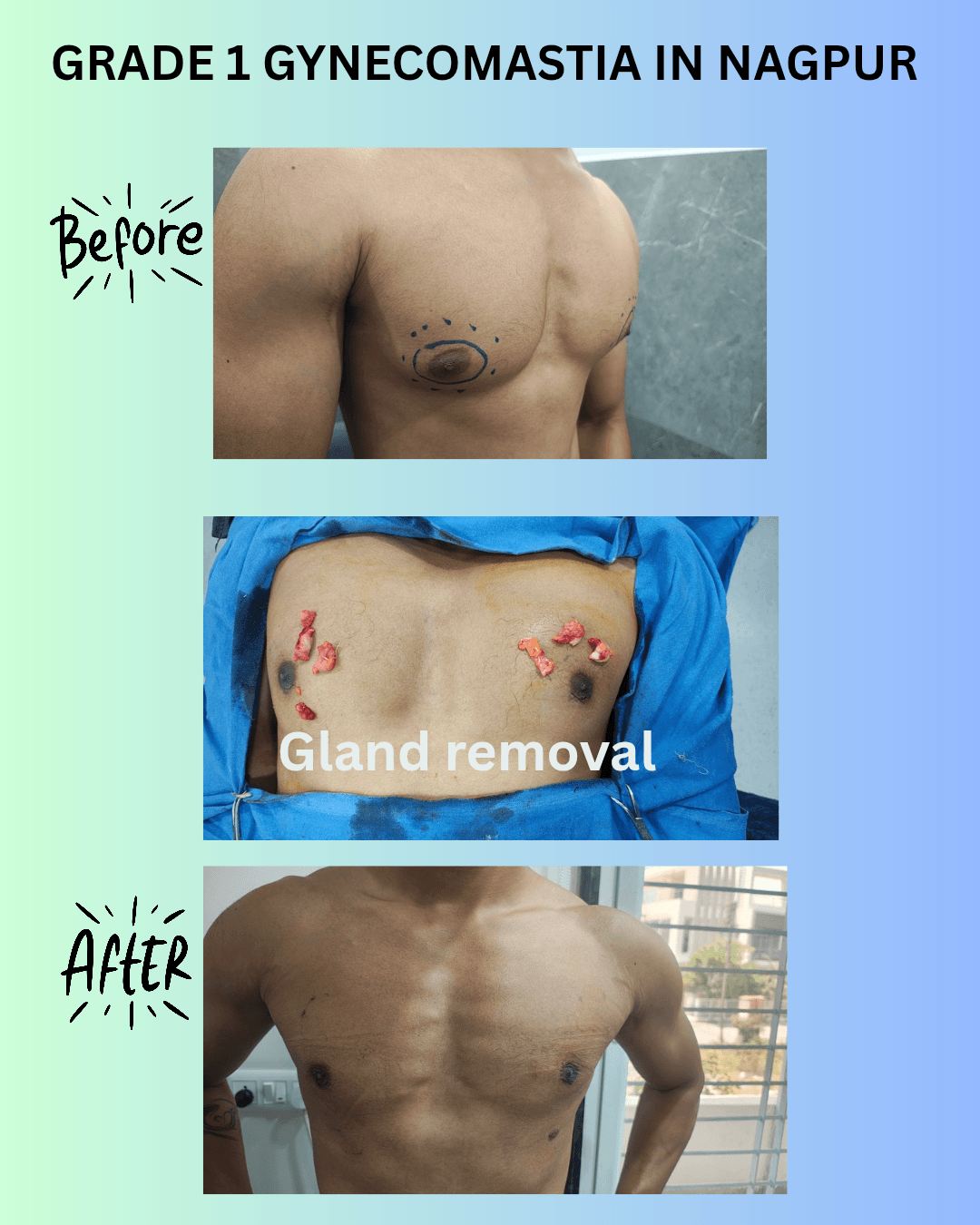
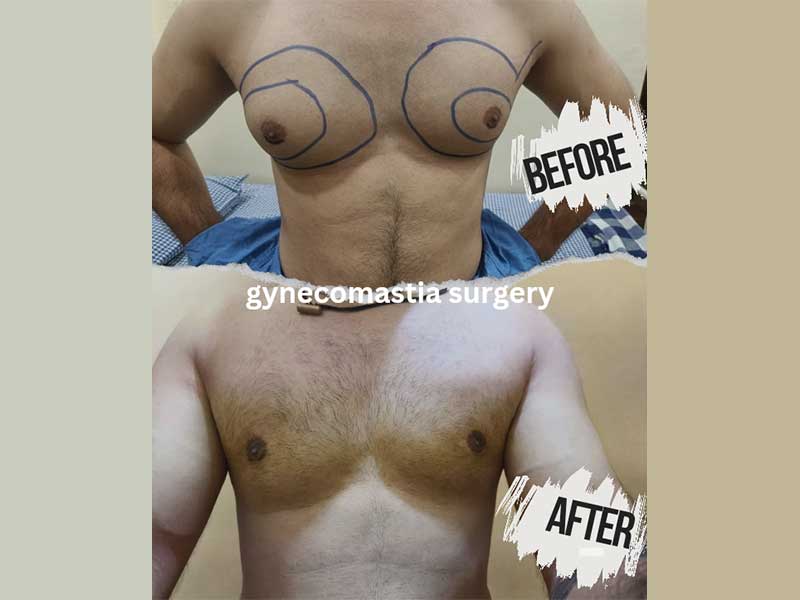
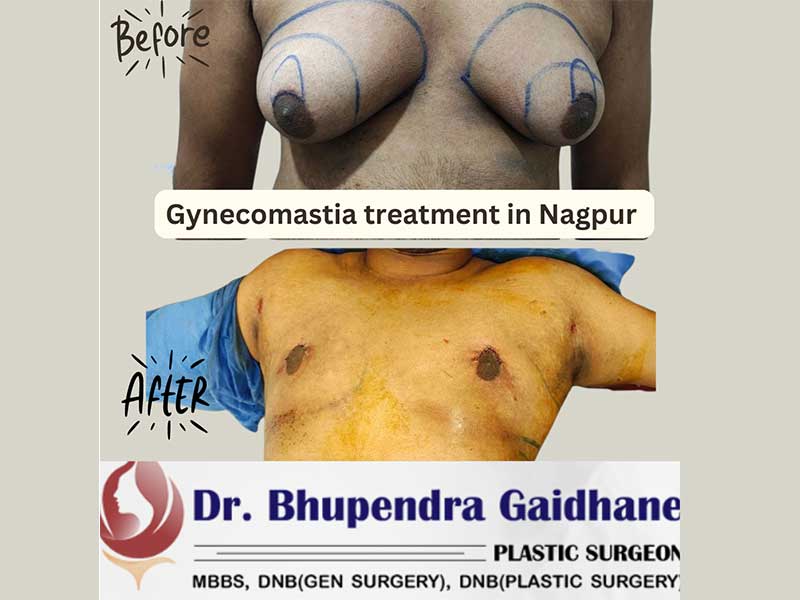
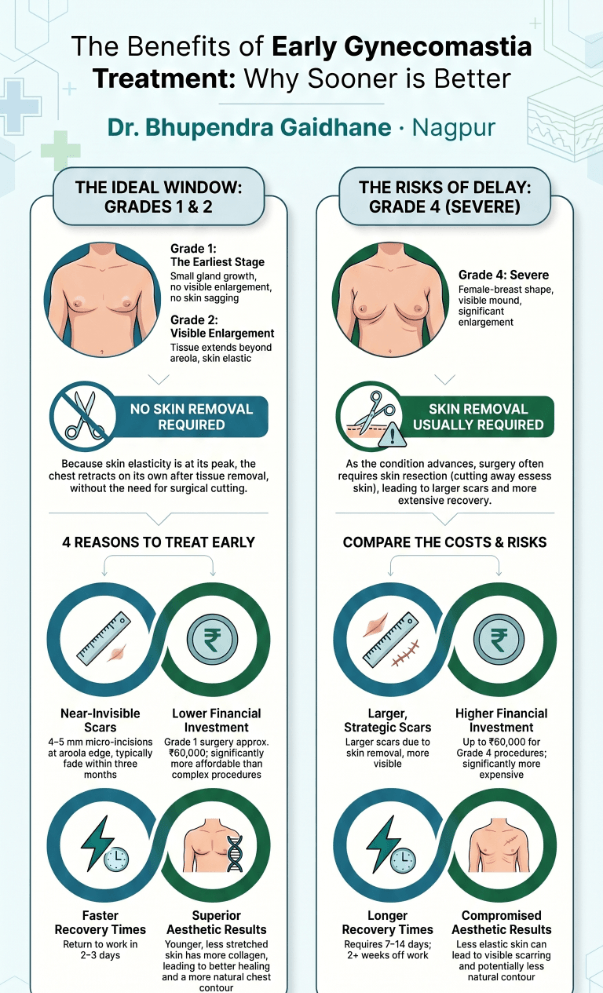
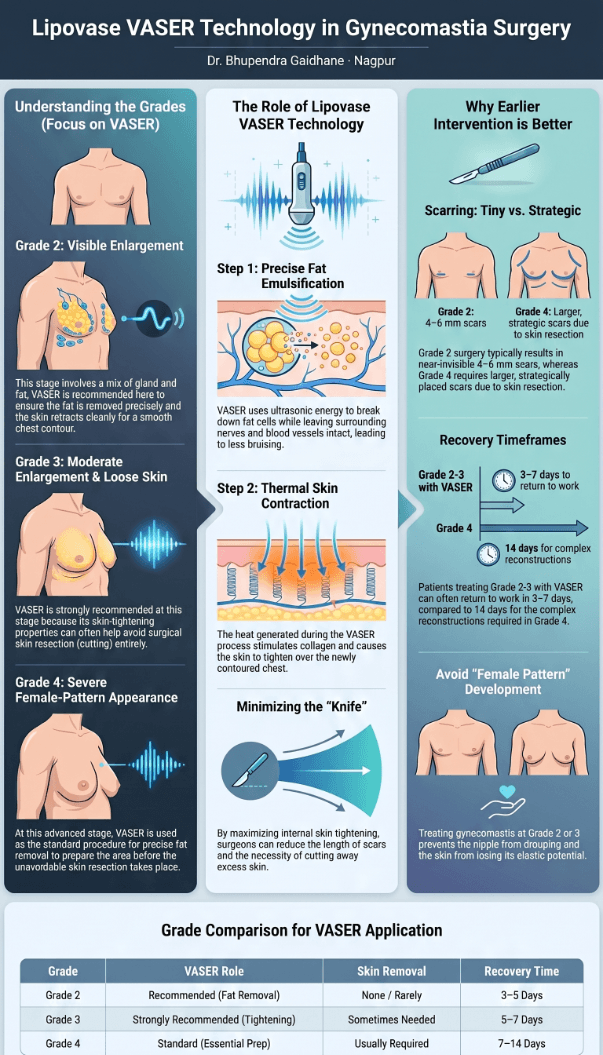
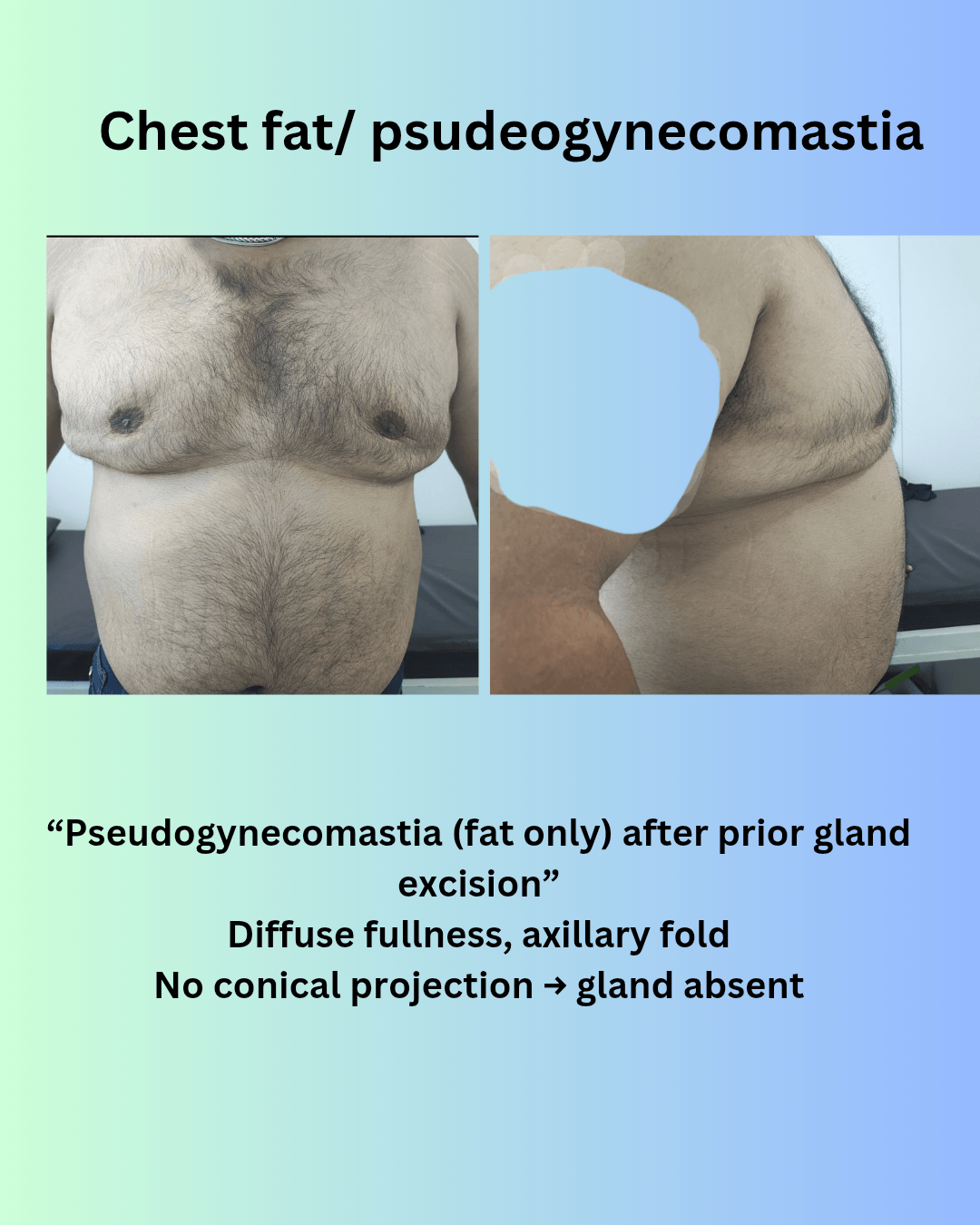
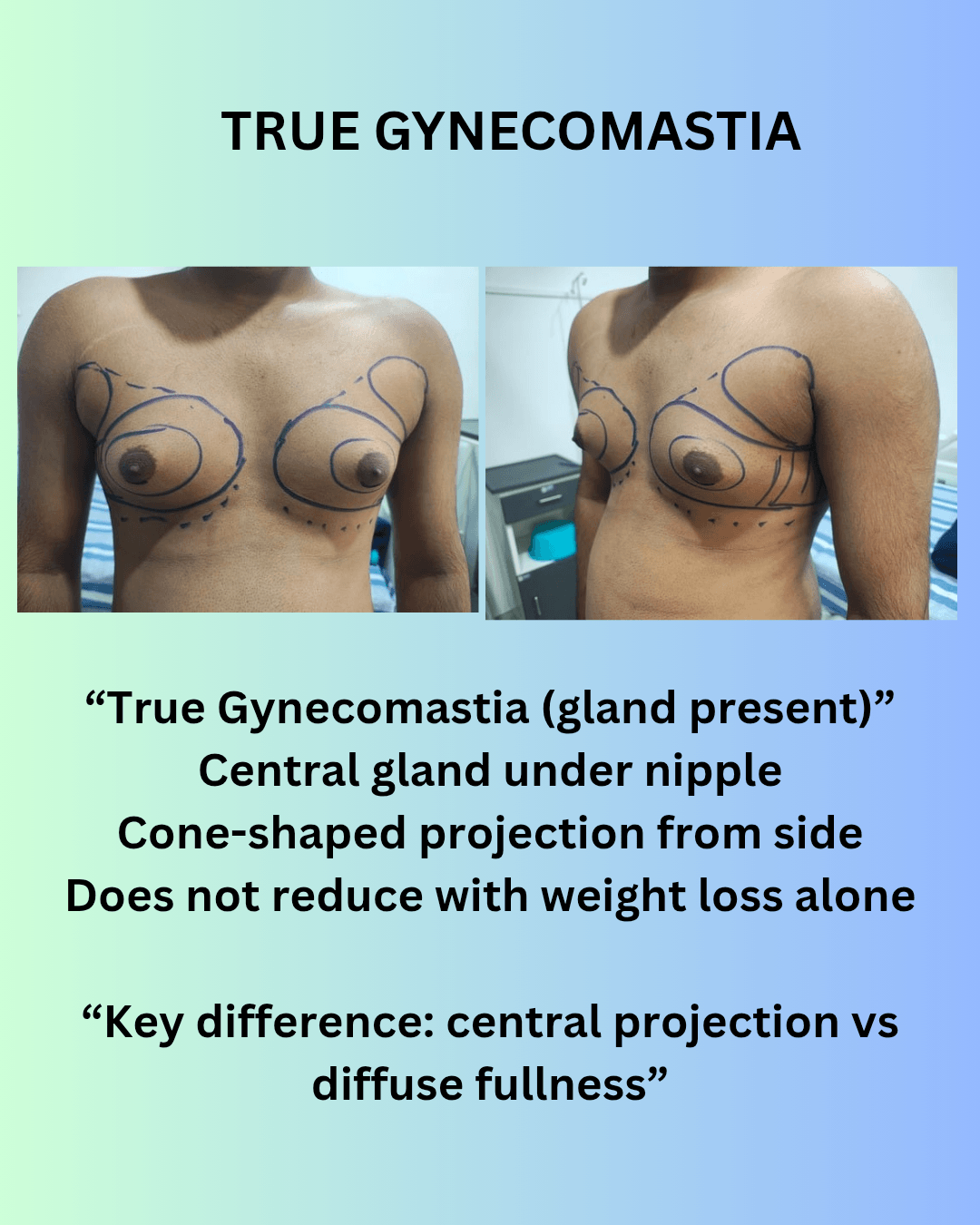
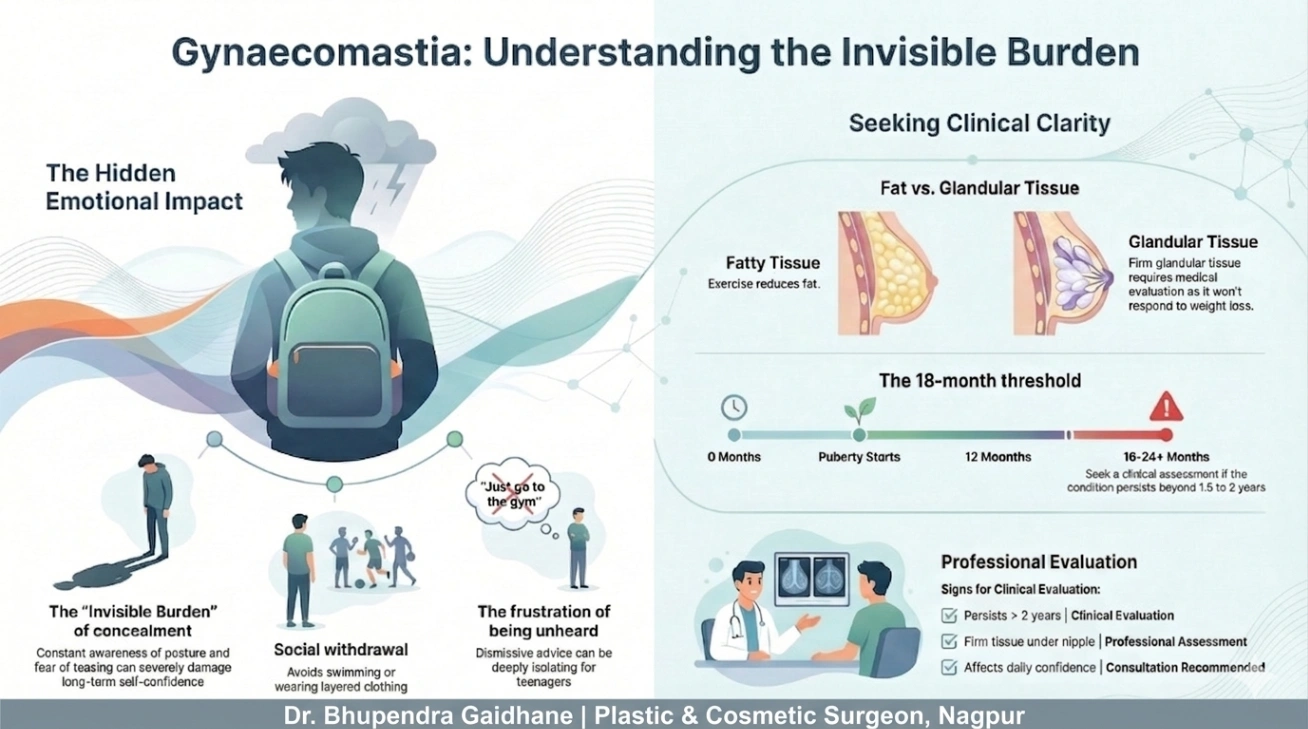
See also: Gynecomastia Surgery in Nagpur — for men dealing with excess chest tissue, a structurally similar decision process applies: fat, gland, and skin each behave differently and require specific correction.
Frequently Asked Questions
Can liposuction tighten loose skin?
No. Liposuction removes fat but does not significantly tighten skin. In patients with existing skin laxity, removing fat without addressing the skin can worsen the appearance. Skin tightening requires a tummy tuck.
Do all women need a tummy tuck after pregnancy?
No — only if skin laxity or muscle separation is present. Some patients with good skin elasticity and minimal fat may do well with liposuction alone. A clinical examination is needed to determine the right approach.
When is the right time for surgery after delivery?
Generally 6–12 months after delivery, after weight has stabilised and breastfeeding has ended. Operating before this point means operating on a body that is still changing — which affects planning and outcomes.
Can liposuction and tummy tuck be combined in one surgery?
Yes. Combining both is common and often ideal — particularly in post-pregnancy and post-weight-loss cases where fat, skin, and muscle are all involved. Both in one session means one anaesthesia, one recovery, and a coordinated result.
Will the gym ever fix my abdomen after pregnancy?
Exercise improves fat distribution and muscle tone — and is valuable for overall health. But it cannot close muscle separation (diastasis recti), and it cannot cause loose skin to retract. If these structural changes are present, no volume of exercise will correct them. That is not a personal failure — it is anatomy.
What about scars from a tummy tuck?
A tummy tuck leaves a horizontal scar in the lower abdomen, placed low enough to be concealed by underwear or swimwear. Scars improve significantly over 12–18 months. Scar visibility and management are always discussed thoroughly before any decision is made.
How is Lipovase different from regular liposuction?
Lipovase uses VASER (ultrasound-assisted) technology to selectively break down fat cells before removal, rather than mechanical disruption. This allows more precise sculpting, smoother contour results, and is particularly effective in 360° body contouring. Traditional liposuction carries a higher risk of irregularity in complex areas.
Ready to find out what you actually need?
If you have been exercising consistently, managing your diet, and are still not satisfied with how your abdomen looks — the answer is a clinical assessment, not more guesswork.
Or call: +91 99609 61451 | drbhupendraplasticsurgeon.com
Dr. Bhupendra Gaidhane
Plastic & Cosmetic Surgeon — Diamond One Building, Dhantoli, Nagpur
Specialising in VASER liposuction (Lipovase), body contouring, gynecomastia, and post-pregnancy restoration.
drbhupendraplasticsurgeon.com | +91 99609 61451