Teenage gynecomastia is more common than most people think. Many boys between the ages of 12 and 18 develop some degree of chest enlargement during puberty.
For some, it settles over time. But for many, it doesn’t.
What is often overlooked is not just the physical condition—but the mental and emotional journey that comes with it.
What Is Teenage Gynecomastia?
Gynecomastia refers to the development of glandular breast tissue in males. During puberty, hormonal fluctuations can temporarily increase estrogen activity relative to testosterone.
This can lead to swelling under the nipple area.
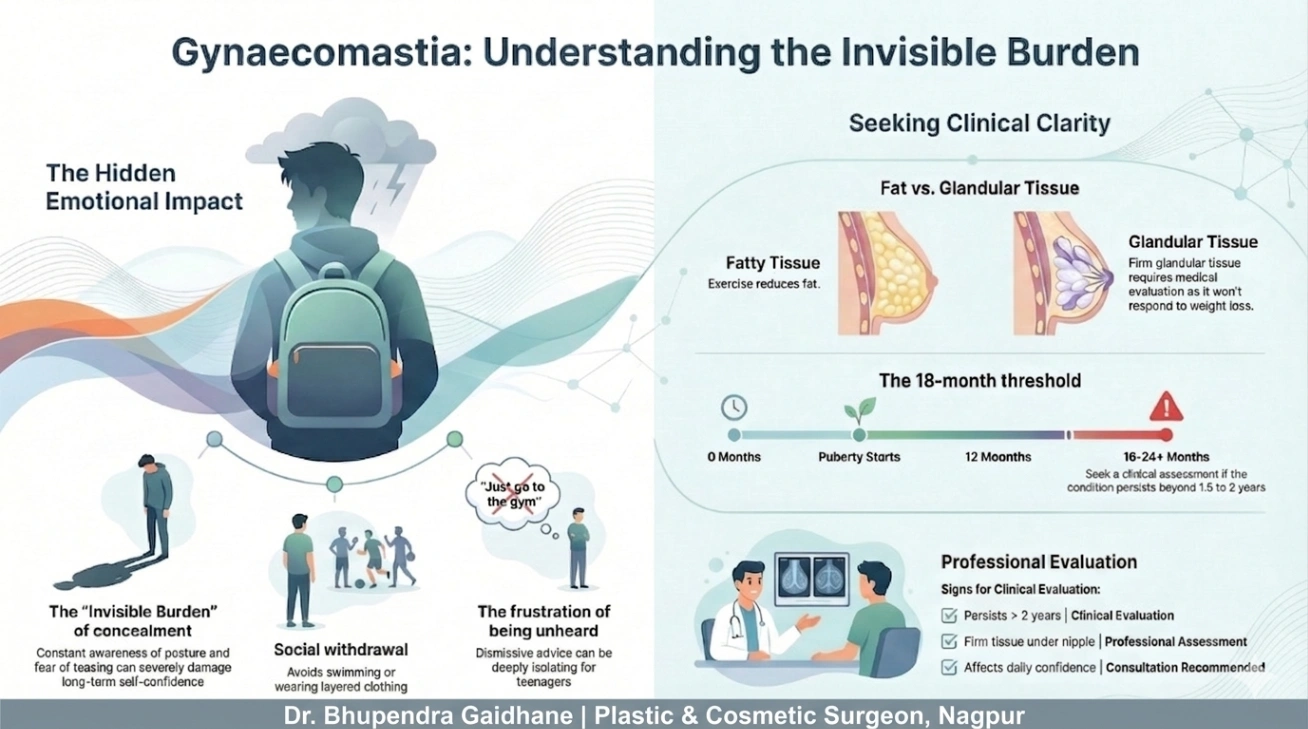
In some cases, it is just fat (pseudogynecomastia). In others, it is firm glandular tissue—or a combination of both.
Understanding this difference is important, because not all chest enlargement responds to exercise or weight loss.
Chest Fat or Gynecomastia? Understanding the Difference
| Feature | Pseudogynecomastia (Fat) | True Gynecomastia (Gland) |
|---|---|---|
| Cause | Weight gain / lifestyle factors | Hormonal imbalance during puberty |
| Texture | Soft, diffuse | Firm or rubbery tissue under nipple |
| Response to Gym | Often improves with weight loss | Usually persists despite exercise |
| Appearance | Reduces as body fat decreases | May remain even after weight loss |
| Management | Diet and exercise | Depends on persistence and evaluation |
This distinction is important because not all chest enlargement responds to exercise alone.
The Reality Most Teenagers Don’t Say Out Loud
A teenage boy with gynecomastia often goes through:
- Avoiding tight clothes
- Wearing loose or layered clothing even in heat
- Avoiding swimming, sports, or changing rooms
- Constant awareness of posture and chest appearance
- Fear of being noticed or teased
Over time, this becomes more than a physical concern. It becomes a confidence issue.
“It Will Go Away” — And the Frustration That Follows
Many teenagers finally gather the courage to speak to their parents.
But they often hear:
- “It’s just fat, go to the gym”
- “You’re lazy, start running”
- “It’s normal, it will go away”
Even during medical consultations, some are reassured without detailed evaluation.
While this may be appropriate in early cases, it does not help when:
- The condition has persisted for years
- There is firm glandular tissue
- The psychological impact is significant
Not being heard often becomes more frustrating than the condition itself.
A Note to Parents
If your son has brought this up, it likely took courage.
Many teenagers hesitate for months or years before speaking about it. By the time they do, the concern is already affecting their confidence and daily life.
Even if it turns out to be temporary, the emotional impact is real in the present.
Listening without dismissing the concern is the first step.
A clinical evaluation does not mean immediate treatment—it simply provides clarity.
Does Teenage Gynecomastia Go Away?
In early puberty, yes—it often can.
But clinical evaluation becomes important if:
- Persistence beyond 1.5–2 years
- No reduction over time
- Firm tissue under the nipple
- Noticeable asymmetry
- Affecting confidence or daily life
 Not all cases need immediate treatment. Understanding when to observe and when to seek evaluation helps guide the right decision.
Not all cases need immediate treatment. Understanding when to observe and when to seek evaluation helps guide the right decision.
Why Waiting Too Long Can Backfire
Here’s the thing most parents aren’t told:
Delaying surgery can make things more complex.
What may seem mild now… can progress to:
- Larger, firmer glands that don’t shrink
- Stretched or sagging chest skin
- The need for skin removal surgery later (larger scars, higher cost)
- More emotional damage — social anxiety, isolation, and low self-esteem
📉 Late intervention = more trauma + more expense + longer healing
📈 Early intervention = minimal scars + lower cost + better results.
| Factor | Early (16–19 yrs) | Late (25+ yrs) |
|---|---|---|
| Incision Size | Minimal | Larger |
| Skin Quality | Tight, elastic | Loose, stretched |
| Recovery | 3–5 days | 1–2 weeks |
| Cost | Lower | Higher |
| Emotional Healing | Faster | Slower |
| Need for Skin Removal | Rare | Often |
When Surgery Is Worth Considering
If the glandular tissue has not reduced in 2 or more years, or if the teenager is clearly struggling with body image, a surgical consultation is appropriate. The ideal age window is 16 to 19 years — at this stage, skin elasticity is high, recovery is faster, and results tend to be cleaner with minimal scarring. Surgery done during a school vacation allows teens to return to normal social life without disruption.
Why Exercise Doesn’t Always Help
Exercise can reduce fat. But glandular tissue does not respond to gym or weight loss.
This is why many teenagers improve fitness but still notice chest prominence.
What Many Parents Realize Later
During surgery, when the glandular tissue and fat are shown, many parents are surprised.
A common reaction is:
“We didn’t realize this was the reason… we thought it was just fat.”
This highlights how often the condition is misunderstood.
When to Consider Evaluation
A proper clinical assessment helps determine:
- Whether it is fat, gland, or both
- Whether it is likely to resolve
- What options are appropriate

Treatment Approach (Overview)
Management depends on the tissue type and severity.
Options may include:
- Liposuction for fat component
- Glandular excision when required
- Combination approach for contour balance
The goal is a natural chest contour with proper planning.
Internal Resources
For more detailed information, you can also read:
faqs
Q: Is gynecomastia surgery safe for teenagers? Yes. It is a short daycare procedure performed under general anesthesia. Teenagers typically recover faster than adults, with most resuming light activity within 3–5 days.
Q: Will there be visible scars? With VASER-assisted micro-incision technique, incisions are 4–6 mm and placed in hidden areas — the areolar margin or armpit. These typically fade to near-invisible within 6–12 months.
Q: What is the downtime for a teenager? Most teens can return to school within 3–5 days. Sports and gym should be avoided for 3–4 weeks.
Q: Can gynecomastia return after surgery? Once the glandular tissue is removed and body weight remains stable, results are permanent. Recurrence is uncommon when the underlying hormonal cause has resolved.
Conclusion
Teenage gynecomastia is not always a condition that needs immediate treatment.
But it is also not something that should be ignored when it persists.
The right approach lies in:
- Knowing when to wait
- Knowing when to evaluate
- Listening to the patient
Consultation
If you or your child is dealing with persistent chest swelling, a clinical consultation can help clarify the situation.
Prime Polyclinic, Dhantoli, Nagpur
Call: 9960961451